Representatives of state and national education groups are refraining from taking a position on whether states should require a new vaccine for cervical cancer for preteen girls, although some say it could be a burden for schools to enforce such mandates.
Seventeen states and the District of Columbia have legislation pending to make the vaccine mandatory, according to the Denver-based National Conference of State Legislatures. And Texas Gov. Rick Perry signed an executive order Feb. 2 requiring 6th grade girls to get a three-shot vaccine to protect them against the human papillomavirus, or HPV, a sexually transmitted disease that causes the majority of cases of cervical cancer.
While Texas is the first state to enact a mandate for the vaccine, Virginia’s House and Senate both have passed bills requiring the vaccine and referred them to committees for further consideration. Most, but not all, state legislative proposals include an opportunity for parents to opt out.
Representatives of some major school organizations have been noncommittal on whether states should require the vaccine; neither the Alexandria, Va.-based National School Boards Association nor the Washington-based Council of Chief State School Officers has taken a stand on the issue.
“We’re not going to take a position on the medical merits here or the process question of whether this is how the legislature or governor should do it,” said Tom Hutton, a staff lawyer for the National School Boards Association. “Schools have to check vaccinations anyway, so if the state decides in its wisdom that this is one more that needs to be required, it’s not that big of a burden.”
Merck’s Role
In Texas, Dax Gonzalez, the communications manager for the Texas Association of School Boards, said “we … haven’t figured out what to do” about Gov. Perry’s mandate.
Any state legislation requiring the vaccine that is enacted would benefit Merck & Co., based in Whitehouse Station, N.J., which is the only drug company with an HPV vaccine on the market. The three-shot regimen costs $360.
A number of states and the District of Columbia have legislation pending that would require pre-teenage girls to be vaccinated for human papillomavirus, or HPV. In Texas, the governor has issued an order requiring vaccination.
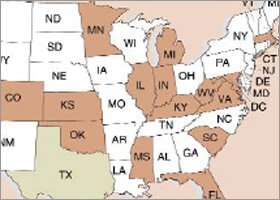
SOURCE: National Conference of State Legislatures
In June, the Advisory Committee on Immunization Practices of the Centers for Disease Control and Prevention in Atlanta recommended the vaccine in females ages 9 to 26. Since then, Merck has been lobbying states to approve laws requiring it, according to news reports. Merck did not reply to requests for comment from last week.
A Feb. 5 report by the Helena, Mont.-based Institute on Money in State Politics shows that since 2000, Merck has given $2.46 million to state-level candidates and party committees around the country. The report mentions that Gov. Perry, a Republican, has received $21,000 to date from the drug company’s political action committee.
Krista Moody, a spokeswoman for the governor, said last week that Gov. Perry made the executive order, rather than waiting for the issue to play out in the legislature, where two bills have been introduced, because “the governor didn’t want to waste any time now that this vaccine is on the market” in preventing cancer.
Concerns Voiced
Some consumer groups and conservative organizations have spoken out against such mandates. The New York City-based Center for Medical Consumers, for instance, contends that the vaccine is too new and hasn’t been studied sufficiently to be considered safe for preteens. Focus on the Family, in Colorado Springs, Colo., supports universal availability of the HPV vaccine but opposes state mandates, contending they violate parental rights.
Some school health professionals say that while they believe the HPV vaccine has merit, they are opposed to schools’ being given the sole responsibility to carry out mandates for it. (“Vaccination Policies Fall on Schools’ Shoulders,” Jan. 24, 2007.)
“It’s an excellent vaccine. It’s going to save lives,” said Dr. Linda M. Grant, the medical director for the 57,000-student Boston public schools and a member of the American Academy of Pediatrics’ Council on School Health. “The whole village has to get involved in this one. School systems need support to carry it out.”
For example, she said, school districts shouldn’t be alone in bearing the financial cost of hiring staff to collect data and produce the reports that schools must keep on hand about students’ immunizations for state auditors.
Marcia Rubin, the director of research for the American School Health Association in Kent, Ohio, had similar concerns about implementation, though she emphasized that schools stand ready to enforce whatever the law requires concerning immunizations.
“It’s very challenging for schools to verify that everyone has the recommended immunizations and the records are complete,” she said. “School nurses have tremendous challenges just to do school nursing, let alone track down immunization records.”
In Maryland, a state legislator who had introduced a requirement for the HPV vaccine withdrew it after concluding that school officials had enough trouble enforcing mandates already on the books for other vaccines. (“Lawmaker Withdraws a Bill Mandating HPV Vaccinations,” Feb. 7, 2007.)
Dr. Grant noted that states typically require vaccines before children can enroll in schools for illnesses including diphtheria, tetanus, whooping cough, hepatitis B, polio, measles, mumps, and rubella.
![Teachers talk during lunch in the teacher’s lounge at Annunciation Catholic School in Minneapolis, Minnesota on Tuesday, May 5, 2026. ] LEILA NAVIDI • leila.navidi@startribune.com](https://epe.brightspotcdn.com/dims4/default/adfdcac/2147483647/strip/true/crop/3537x2400+32+0/resize/840x570!/quality/90/?url=https%3A%2F%2Fepe-brightspot.s3.us-east-1.amazonaws.com%2F4a%2F27%2Fa71ae6c64cbe887f40d2c3e1a063%2Fus-news-minn-annunciation-teachers-year-filepic-5-ms.jpg)



